What is Mucosal Cancer?
What is Mucosal Cancer?
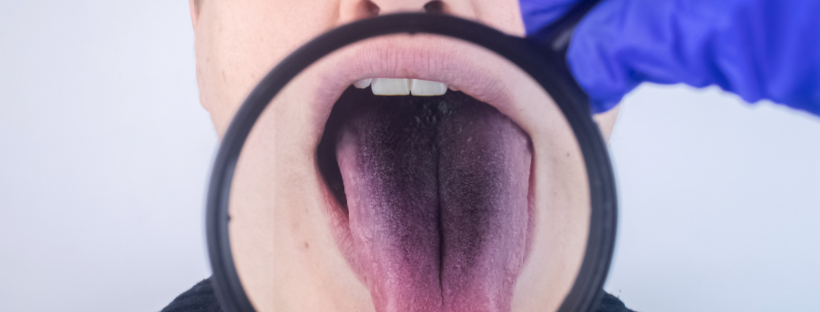
Mucosal cancer, also known as mucosal carcinoma, refers to a type of cancer that develops in the mucous membrane lining various parts of the body.
The mucous membrane, also called the mucosa, is a thin, protective layer that covers the surface of organs and body cavities, such as the mouth, nose, throat, lungs, stomach, and intestines.
Melanoma develops if there is uncontrolled growth of melanocytes, the cells responsible for pigmentation. The majority of melanomas are cutaneous, ie they grow within the skin.
Mucosal melanoma is a rare type of melanoma that occurs on mucosal surfaces. Mucous membranes are moist surfaces that line cavities within the body. This means that mucosal melanoma can be found in the respiratory tract, gastrointestinal tract or genitourinary tract.
Mucosal melanomas are most often found in the head and neck, in the eyes, mouth, nasopharynx and larynx, but they can also arise throughout the gastrointestinal tract, anus and vagina
The causes of mucosal cancer can vary, but certain factors such as smoking, excessive alcohol consumption, a family history of cancer, exposure to certain chemicals or toxins, and certain infections, such as human papillomavirus (HPV), can increase the risk of developing mucosal cancer.
Symptoms of mucosal cancer may include difficulty swallowing, persistent coughing or hoarseness, changes in bowel or bladder habits, unexplained weight loss, and pain or discomfort in the affected area.
They make up approximately 1.1% of all melanomas but are usually more complicated because of late diagnosis due to their less visible locations and because they are often amelanotic – meaning they are not pigmented.
Treatment options for mucosal cancer may include surgery, radiation therapy, chemotherapy, or a combination of these approaches, depending on the location and stage of the cancer.
Which parts of the body are affected by mucosal melanoma?
Subtypes of mucosal melanoma are based on the tissue in which they arise. Melanoma can start within any mucosal epithelium. The most common sites are:
- Respiratory tract
- Nasal cavity
- Paranasal sinuses
- Oral cavity
- Gastrointestinal tract
- Transitional zone of anal canal (the line where the normal skin meets the mucous membrane)
- Genitourinary tract
- Vulva
- Vagina
Who gets mucosal melanoma?
The peak age of diagnosis of mucosal melanoma is between 70 and 79. However, younger people have also been known to develop mucosal melanoma, especially of the oral cavity.
Mucosal melanoma of the genital tract is more common in females.
What causes mucosal melanoma?
While there are many suggested risk factors for mucosal melanoma, there is only weak evidence for all, and none that are widely accepted.
About 25% of mucosal melanomas have been linked with problems with a gene called KIT.
Genes are the templates used for making protein, and mutations in the KIT gene cause the production of a mutant protein.
The KIT gene can also be over-expressed, which means that there is more of the KIT protein being made than usual.
Both the mutation and over-expression of the KIT gene have been associated with mucosal melanoma.
Possible risk factors include:
Oral mucosal melanoma
- Smoking
- Ill-fitting dentures
- Ingested/inhaled environmental carcinogens
Vulvar melanoma
- Chronic inflammatory disease
- Viral infections
- Chemical irritants
- Genetic factors
Anorectal melanoma
What are the signs and symptoms of mucosal melanoma?
The signs and symptoms of mucosal melanoma largely depend on its location. Therefore, there are a wide variety of symptoms that patients may experience.
Mucosal melanoma of the head and neck
- Discolouration in the mouth
- Painless bleeding lump
- Ulceration
- Ill-fitting dentures
- Nasal obstruction
- Nose bleeds
- Loss of smell
Vulvovaginal melanoma
- Discolouration of the vulva
- Itch
- Bleeding
- Discharge
- Ulceration
- A mass
- Pain during/after intercourse
Anorectal melanoma
- Bleeding
- A mass
- Anal or rectal pain
- Change in bowel habit (such as constipation or diarrhoea)
What is the treatment for mucosal melanoma?
The best form of treatment for mucosal melanoma is wide local excision of the lesion.
This may not always be possible, as the melanoma may be located on an important anatomical structure, or be too large to excise safely.
Due to the likelihood of the same melanoma recurring, surgical resection is often combined with radiotherapy.
Radiotherapy is also a consideration for patients who are not suitable for surgery.
What is the prognosis for mucosal melanoma?
Mucosal melanomas have a poor prognosis, as most patients develop metastases despite aggressive therapy.
The typical mucosal melanoma 5-year survival rate:
- Head and neck 12-30%
- Vulvovaginal / Vulval 24-77%
- Vaginal 5-25%
- Anorectal 20%
More Skin Tips.
CoreBodi







| Powered by Kaptol Media


